 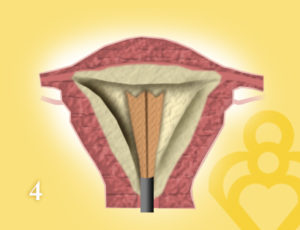
These options have become popular due to the ease of use, safety, and similar outcomes to resectoscopic techniques. Second-generation techniques include thermal fluid, microwave or bipolar radiofrequency electrical energy, laser thermotherapy, and cryoablation. The devices used are global and treat the whole endometrial cavity. Many devices that do not require the use of a resectoscope are currently available to accomplish the destruction of the endometrium. 
The major disadvantage to resectoscopic endometrial ablation is operator expertise and safety. The endometrium is desiccated to the level of the basalis layer using thermal energy. This technique is performed under hysteroscopic guidance using a rollerball, monopolar, or bipolar loop electrode. Both techniques insert a device into the endometrial cavity and use different methods or energy to injury the endometrial lining. Two techniques are described for endometrial ablation: resectoscopic and non-resectoscopic. Before performing an endometrial ablation, a benign endometrial biopsy must be obtained. This information can be obtained by a preoperative transvaginal ultrasound or saline infusion sonogram. Lastly, the anatomy of the uterus is an important consideration, including the length of the cavity (no larger than 11cm) and contour of the cavity. The ideal patient has AUB related to the endometrium as determined by the FIGO classification system and does not desire definitive management with a hysterectomy. Further criteria should include AUB that is not related to a structural cause, hyperplasia or malignancy, and failure or intolerance of medical management. Candidates for endometrial ablation include women of reproductive age who have met their desired parity with heavy menstrual bleeding due to a benign cause that significantly impacts their quality of life. Īppropriate patient selection is important for the treatment of abnormal uterine bleeding with endometrial ablation. After endometrial ablation, necrosis, fibrosis, and inflammation are common histology findings of the uterine cavity. By destroying these layers, the endometrium is no longer able to regenerate, thereby causing menstruation suppression. The various endometrial ablation techniques destroy the endometrial lining, removing both the functional and basal layers. The functional layer performs the physiologic functions of proliferation, maintenance of pregnancy, and menstruation, while the basal layer is implicated in regrowth of the functional layer. 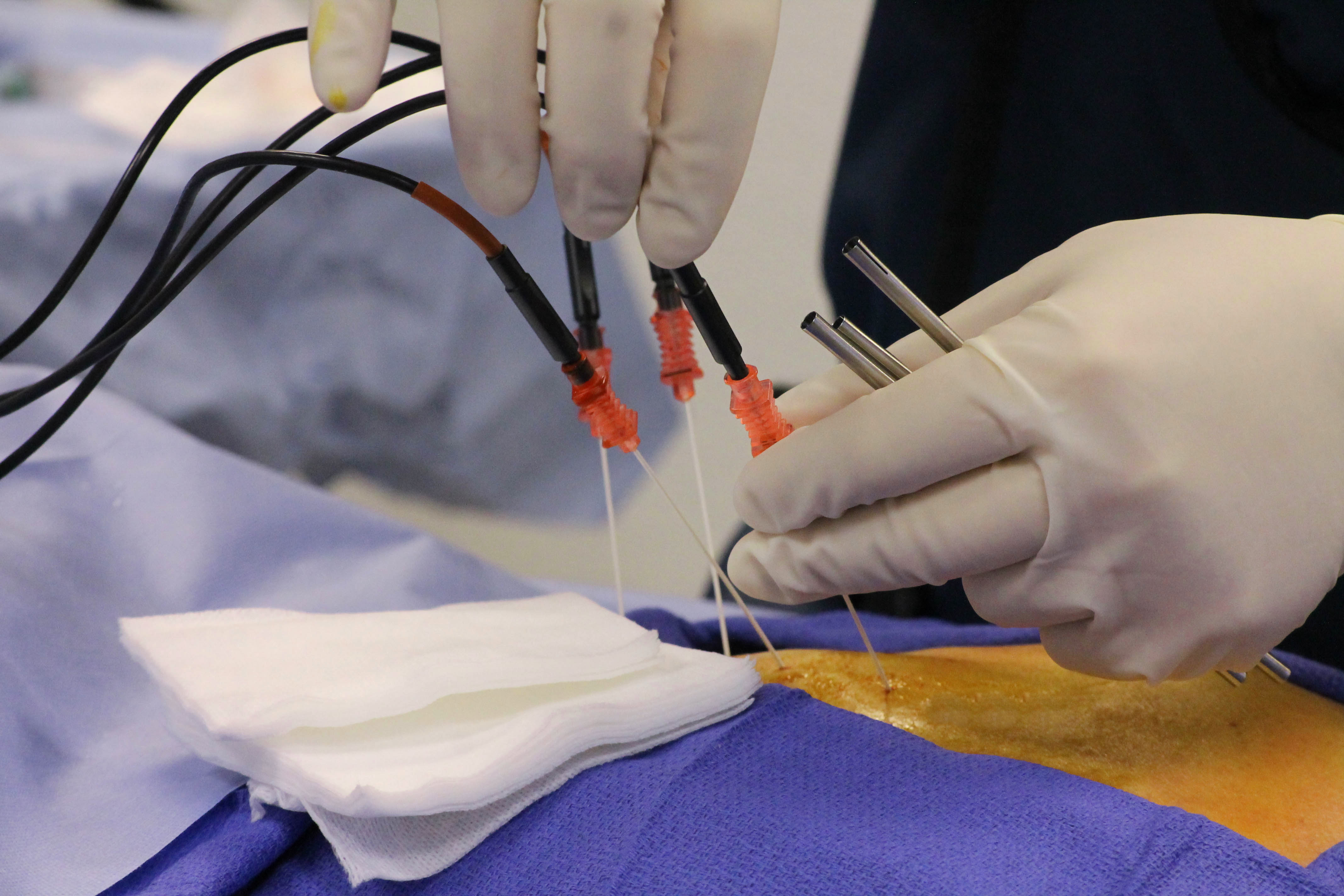 
The endometrial lining of the uterine cavity is composed of a functional and basal layer. Endometrial hyperplasia or malignancy is an underlying cause of abnormal uterine bleeding and needs to be evaluated before an endometrial ablation with a histological sample of the endometrium. Non-structural causes of AUB can be due to endocrinopathies, underlying bleeding disorders such as von Willebrand disease, or iatrogenic causes, including various contraceptive methods or medications such as anticoagulants. Ī transvaginal ultrasound, saline infusion sonogram, or hysteroscopy are used to determine structural abnormalities and provide information on the size and position of the uterus. The non-structural causes of abnormal bleeding include coagulopathy, ovulatory dysfunction, endometrial, iatrogenic, and not yet classified. There are structural causes of abnormal bleeding, including polyp, adenomyosis, leiomyoma, or malignancy. There are many different causes of AUB, which can be classified by the acronym PALM-COEIN, a universally accepted nomenclature that was developed by the International Federation of Gynecology and Obstetrics (FIGO). Prior to performing endometrial ablation, it is important to evaluate the etiology of abnormal uterine bleeding to determine the correct management. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
